Eczema affects millions of people across the world. While the exact causes of eczema aren’t always completely clear, your genes may play a role. So, is eczema genetic? We’ll find out below.
Introduction to Eczema and Genetics
Who here is familiar with the “Atopic March”? No, it’s not an obscure piece of music written by an even more obscure composer. It’s the unsightly parade of eczema, asthma, and allergies, an event you couldn’t be paid enough to attend. The intro to this terrible tune, eczema (eg-zuh-MUH), plays across the entire lifespan from infancy through adulthood. As you might expect, this would make a genetic connection highly likely, but is eczema hereditary?
If you live with eczema, then you know how tough it can be to soothe your symptoms on a daily basis. Eczema is a condition that causes symptoms like itching and red, inflamed skin. People often wonder if eczema is contagious, because it can turn into what looks like growths on the skin, but it’s just something in the environment interacting with a person’s skin and a dysfunctional immune response.
Eczema is also rather common. Up to 1 in 3 children experience it, usually in the first year of life, but it can last into adulthood. It might vanish for years and then abruptly flare up, because it can be caused by a wide variety of things. It’s less common (2-10%) in adults, but still affects millions [1].
Unsurprisingly, a major player when it comes to eczema is genetics. Genes involved in eczema may influence [2, 3, 4, 5, 6, 7]:
- Skin barrier function
- Inflammation
- Immune response
Types of Eczema
Eczema is an unfortunate combination of dysfunctional skin barrier and immune response [8]. It lets bad things in and lets water out.
The most common form of eczema is atopic dermatitis, which is basically an allergic skin reaction to some kind of allergen. This is why in adults, eczema is more common in rural communities, as people tend to be out in the environment more doing things with their hands.
People who have eczema have greater odds of also having asthma, and/or hay fever [1]. They all have similar, underlying immune response mechanisms.
It might surprise you though, to find out that there are actually 7 different types of eczema. They include the following [9]:
- Atopic dermatitis is the most common type and is an inflammatory immune response to an allergen of some kind, can be infected with staph, and need treatment to be cleared.
- Contact dermatitis is an inflammatory (but not immune) response to skin damaged by some form of irritant. A good example is poison ivy.
- Neurodermatitis is often derived from other forms of dermatitis, involving small areas of very itchy skin that get scratched excessively, forming tough, leathery patches of skin.
- Dyshidrotic eczema forms small, itchy blisters, usually on the hands and feet, and tends to run in families.
- Nummular eczema forms circular shaped, sometimes oozing patches, often infected with staph that needs treatment to be cleared.
- Seborrheic dermatitis is commonly seen with “cradle cap” in babies, affects areas with more oil-producing glands, and is a common reaction to too much of a particular yeast that lives on the skin.
- Stasis dermatitis more often affects older people and is a result of poor circulation in the lower extremities, causing itchy, scaly skin and red spots due to burst capillaries.
What Causes Eczema Flare Ups?
One of the difficult parts of managing eczema is identifying the environmental triggers that cause flare-ups. For a lot of people, simple allergy tests with their dermatologist will do the job.
But for some people, these triggers can be difficult to determine. You move, get a new job, get older, all of which can alter your environment and bring you into contact with things that may trigger eczema. It’s an ongoing effort, and sometimes you won’t know something is a trigger until the eczema flares up.
Some environmental elements that can make the symptoms of eczema worse include [10, 11]:
- Contact with allergens (pollen, mold, dust mites, or animals)
- Cold, dry air
- Infections like the flu
- Contact with skin irritants (chemicals or fabrics)
- Stress
People with eczema may also be more prone to skin infections due to having a compromised skin barrier [1, 12].
There is no magic pill to prevent eczema. Figuring out and avoiding triggers are the best methods for not getting it, but sometimes life isn’t that easy so symptom management becomes the only option. The symptoms of eczema can usually be managed at home with the help of [13]:
- Moisturizers
- Humidifiers
- Topical medications
- Trimming or covering fingernails (to limit scratching)
- Avoiding skin irritants
When it comes to finding soothing techniques to help with troublesome triggers, there may be a genetic element. If you’re struggling to identify your eczema triggers, your genes might provide some clues to solve the mystery. These triggers differ from person to person and can include certain fragrances, metals or fabrics [1, 14].
While there isn’t a completely clear cause of eczema, genetics seems to play a major role. What’s more, the genetics of eczema, asthma, hay fever, and food allergies are very similar. This means that if you have one, you’re more likely to have the others [10, 15].
Is Eczema Genetic?
We’ve seen that eczema involves three major elements: skin barrier, inflammation, and immune response. So, it makes sense that genes involved in these elements would affect your risk level for not only getting the condition, but the severity as well. In fact, up to 75% of differences in people’s chances of developing eczema may be attributed to genetics [2].
We’ll look at a gene for each of these areas, but understand that there are numerous genes involved [4, 5, 6]. So, let’s dive into one important factor when it comes to eczema: genetics.
The FLG gene helps make filaggrin, a protein that’s essential for the skin barrier. Filaggrin mutations create a haphazard organization of the skin cells. This dysfunction causes a ‘leaky’ skin barrier allowing water loss and decreased protection from harmful substances [1].
Because of this, variants of this gene might increase your sensitivity to eczema food triggers. On a positive side, skin moisturizers and colloidal oatmeal may lessen the impact of FLG variants by strengthening your skin barrier [16, 17, 18, 19].
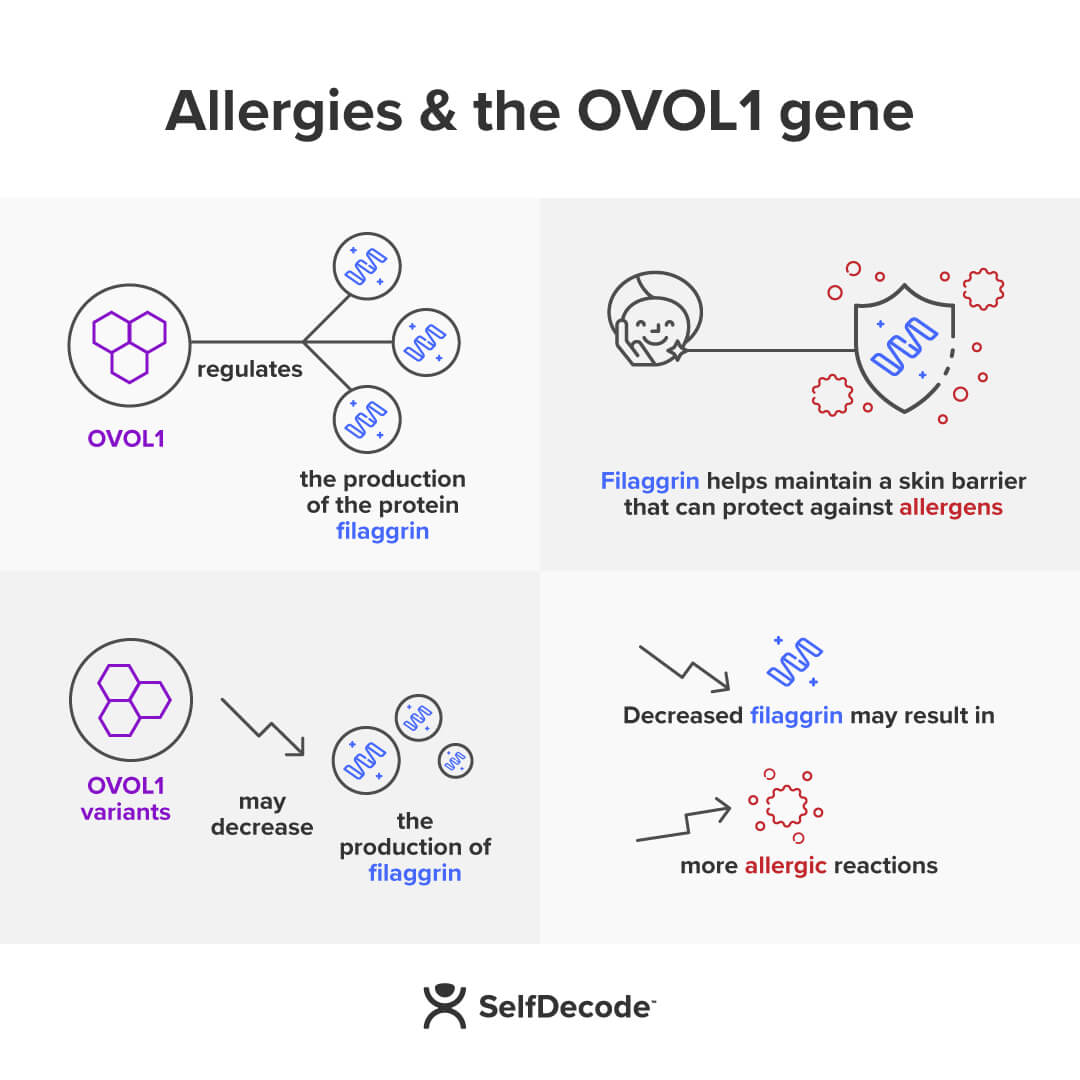
Another gene that can affect your skin barrier is the OVOL1 gene. A variant in this gene may likely impair the skin barrier, increasing your odds of developing eczema [20, 21, 22].
Then there is the HLA-DQA1 gene. The protein made from this gene helps white blood cells distinguish invading cells from healthy ones. Variants here can impair this ability of white blood cells and make it more likely for things to cause infection.
Another example involving eczema and genetics is the IL13 gene. This gene makes interleukin 13, one of the numerous interleukins involved in your immune system. In this case, it functions to limit the expression of filaggrin and generate inflammation. Variants in this gene can increase its effect, making inflammation more likely or worse for people with eczema.
These are just some examples of how genes can influence your skin health. Because a major risk factor for eczema is genetics, knowing your genes may help you manage your flare ups.
How Analyzing Your DNA Can Help With Eczema
Contrary to what you may think, having your DNA analyzed can help you understand what risk factors are relevant to you based on your genes and what you can do to address them.
For example, if you have that certain OVOL1 gene that may increase your odds of experiencing eczema, moisturizing may help you protect the skin barrier.
By analyzing over 7,300 genetic variants, SelfDecode can provide the most accurate genetic risk scores and personalized recommendations to help you optimize your skin health.
The SelfDecode Eczema report allows you to optimize your skin health by uncovering what your genes are doing behind the scenes to affect your odds of struggling with eczema. Finding out if your eczema is genetic is just the first step. By understanding your risks, you can make targeted changes to counteract the negative effects of your genes.
Your SelfDecode report comes with evidence-based diet, supplement, and lifestyle recommendations to help you optimize your skin health. Beyond eczema, SelfDecode also offers DNA reports covering psoriasis, acne, stress, and 30+ other health topics.
Concluding Remarks About Eczema
It’s not just some dry skin, as some would. If you’ve had to or currently deal with this skin condition, you know it can be more than just the physical pain of an eczema flare-up.
One major factor that can influence eczema is genetics, so knowing your predispositions may help you get a head start in identifying your triggers and which strategies may work best for you.
Be proactive and start today by investigating your DNA to discover ways you might better address eczema and understand how your genes may be affecting you, for better or worse. For a gene-based approach, you should check out SelfDecode.
Related
- Is Psoriasis Genetic? What It Is, Triggers & How To Manage
- Is Acne Genetic? How Your Genes May Help Improve Skin Health
- What Is A Genetic Mutation?