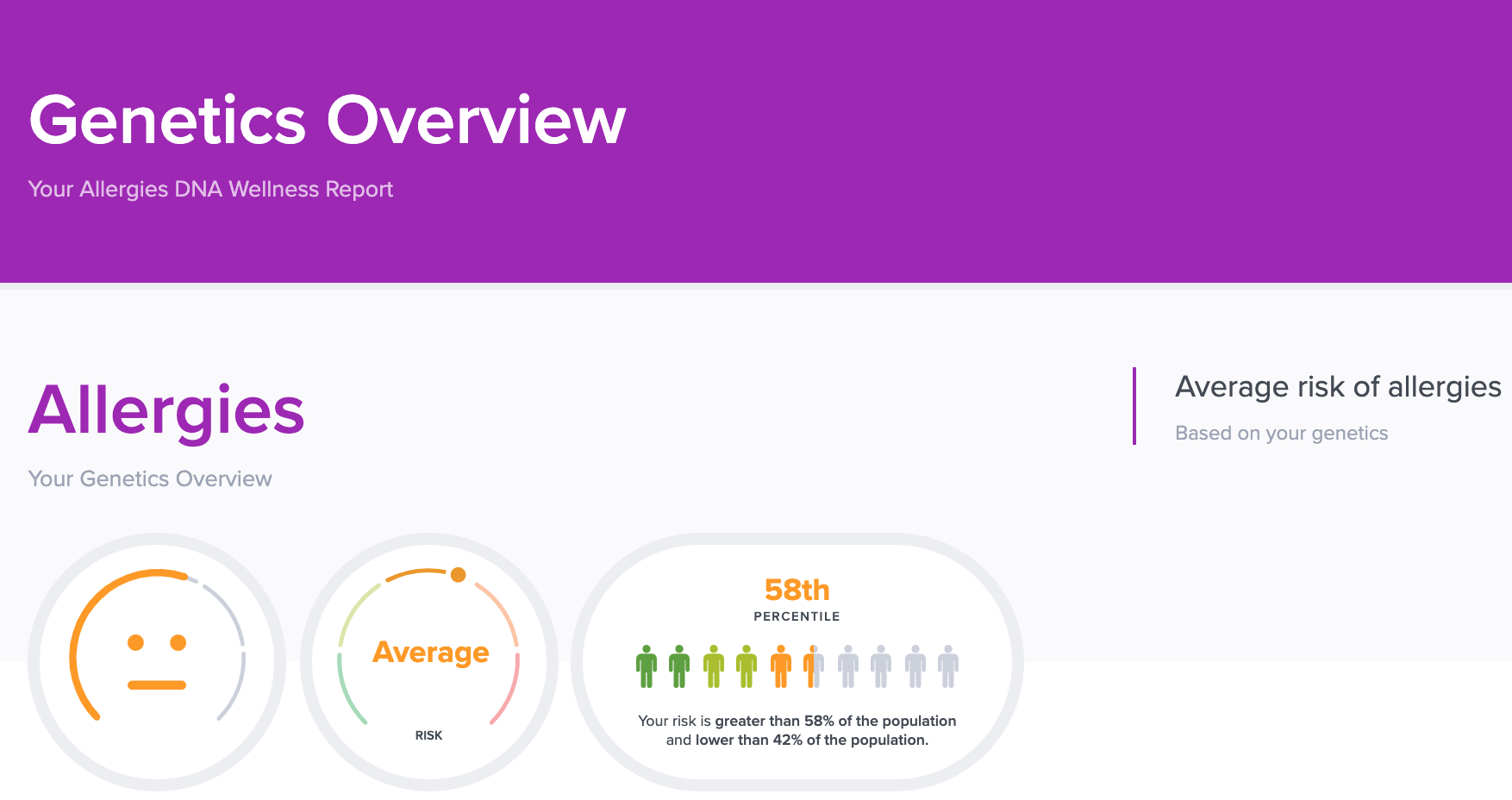
As of 2018, 19.2 million people were diagnosed with hay fever (allergic rhinitis) in the U.S. [1]. It’s the most common respiratory allergy. This is just an allergy to pollen. People can be allergic to all kinds of things. With so many people being allergic to so many things, it can make you ask, are allergies genetic? Yes, genetics can influence your chances of developing allergies. Let’s dig in to find out more!
Introduction To Allergies And Genetics
Somewhere between 10-20% of the world’s population has some sort of allergy to cats and/or dogs. With so many people owning pets, you can imagine that it’s a big problem. But the symptoms you experience are not the only consequence of allergies. In the U.S., if you include lost productivity, it is the costliest disease [2]. So, it’s nothing to, um… sneeze at.
Air pollution, a greater variety of food exposure, chemical agents, are all things over the past century of advancement that have affected an increase in allergies around the world. One category that likely wouldn’t make your list of things to increase allergies would be “botanical sexism”.
What on earth is that, you ask? It’s an odd historical fact of urban policy that led cities to plant mostly male trees instead of females within their city limits [3].
In nature, there is a regulation, a balance between pollen-producing male trees and seed-producing females. Some trees produce both elements.
When city planners back in the mid 20th century began to plant trees to beautify their cities, they wanted to avoid the nuisance of cleaning up the seed production of female trees. This male favoritism inadvertently created a much bigger pollen problem in many city environments around the world.
Thus, decades later, asthma and hay fever in cities has grown significantly, and people are now paying the price. Is this the only reason for it? No, it’s not. Air pollution, chemicals, and other irritants that weren’t a part of our lives in the past are all having an impact.
But is it only your environment, or are allergies? Now, our genes change at a far slower pace than technology. We’re talking 100’s to 1000’s of years and more. The past couple hundred years of development have given our genome little time to adjust, so all it can do now is react to what is presented given the tools it has.
The STAT genes offer a good example of the problem. They are a family of proteins that help regulate immune response. Though variants in all six of them can affect immune response, STAT6 is known to affect allergies.
This heightened response variants in this gene can create is called allergic sensitization [4, 5]. These variants aren’t new to the past few decades. They’ve likely been around for centuries or longer. Society, however, is now introducing factors our genomic toolbox wasn’t set up to deal with.
So, it’s not only your environment that contributes to allergies. Genetics can influence how you respond to these environmental factors. Though to be fair, it’s easier to regulate the causes for allergies than to control our genes.
What Does It Mean To Be Allergic?
At the most basic level, having an allergy is simple to understand. It means your body considers something normally safe to be harmful. These typically safe things are now considered triggers. They trigger your immune system to fight off these “harmful” invaders. This allergy trigger is called an allergen.
The best-known allergens are peanuts and pollen. However, people can be allergic to just about anything. The different types of allergies include [6, 7, 8]:
- Respiratory
- Food
- Contact
The level of response your immune system has to an allergen exists along a continuum from mild to catastrophic. You might step into a room with a cat and start to sneeze uncontrollably or you could eat a peanut and find yourself unable to breathe. While these may seem like completely different sorts of responses, they’re really just different parts of the same process [9].
When you come into contact with an allergen, white blood cells release histamine and other molecules that cause inflammation. This response can build upon itself, cascading into a chain reaction. At its worst is anaphylaxis, which is what can make you unable to breathe. If not responded to quickly, usually with a shot of epinephrine, it can lead to death. However, relative to the number of people with allergies, this kind of allergic response is very rare [10].
The vast majority of people experience mild reactions, like itchy eyes and runny nose or sneezing in the case of hay fever. When these issues are persistent over time, they can cause other problems. These problems could include loss of productivity, loss of sleep, sinus and ear infections, and the worsening of asthma symptoms [11].
So, even mild allergies can lead to ongoing disruptions and lessen the quality of life.
Allergy Testing
Let’s say you’re out working in your yard and find yourself rubbing at itchy eyes or wiping at a runny nose. Or you might find yourself at a friend’s house, petting their three cats, and find you can’t stop sneezing.
If you suspect you’re allergic to something or even concerned about what you or someone you know might be allergic to, you can get an allergy test. These are commonly done with your physician.
The most common types of allergy tests are [12, 13, 14]:
- Skin prick test: The allergen is mixed into water or oil. The doctor places a droplet on your arm and pricks the surface of the skin. If the skin becomes red and swollen, you are having an allergic reaction.
- Patch test: A patch is soaked with the allergen and placed on the skin for 1-3 days. This test is used to find allergies that don’t cause a fast, dramatic reaction.
- Provocation test: In a lab setting, you are exposed to an allergen. If you are testing for seasonal allergies, a doctor may spray specific types of pollen up your nose. This test is only used when other tests haven’t produced clear results.
Dealing With Allergies
Once identified, allergies generally cannot be treated. You don’t “cure” allergies. Your best option is to prevent them from happening in the first place. You may examine every list of ingredients and insist on knowing everything that goes into a restaurant dish. You might avoid jewelry if certain metals give you a skin rash. If prevention is not an option, then you can only work to mitigate the symptoms. [15, 8].
Respiratory allergens are tougher to avoid. If you have seasonal allergies, pollen is everywhere, indoors and out. If you’re sensitive to fragrance, you never know when someone wearing heavy perfume will pass you in the street [16, 17, 18].
What can you do? People with respiratory allergies often look for ways to minimize their reactions. Doctors may recommend medications, lifestyle changes, and nasal cleansing. Yes, nasal cleansing. Pollen irritates the membranes in your nose. Your body thinks it’s an invading germ and generates a sneeze or ten to get rid of it. Some people try supplements or diet changes [19, 16].
With so many things that trigger a reaction, it can be hard managing your allergies. Genetics may play an important role in your risks and what strategies are more likely to have an effect to help you control your symptoms.
Because much of the focus on allergies is on prevention, knowing what you may be predisposed to, whether for allergies, or how severe your reactions might be, can go a long way to help your prevention efforts.
Are Allergies Genetic?
Put simply, the answer to, “Are allergies hereditary?” is, “Yes”. The research tells us that up to 84% of differences in people’s chances of having allergies may be attributed to genetics [20]. This is a strong number.
There are a number of genes that have an effect on our response to allergens. They deal with immune response, inflammation, and skin barrier function [12, 21]. Because we’ve been talking about respiratory allergies here, and how they can cause inflammation, we’ll use a related gene as an example. This gene is called interleukin 13, or IL13.
Interleukins are a major component of our immune systems. They are proteins made in response to pathogens entering the body. There are about 40 known interleukins, whose job is to either promote or inhibit inflammation [22]. Some can do both. Thus, it makes sense that mutations amongst these particular genes could either help or hurt your odds of getting and/or dealing with allergies.
In the case of IL13, we get a “good-guy, bad-guy” situation in the context of asthma. One variant of the gene can be beneficial, allowing for particular medications to work more effectively, whereas another variant can increase the risks of worsening asthma symptoms [23]. Knowing this kind of information can better inform your response to a condition like asthma.
Analyzing Your DNA Can Help You With Allergies
Allergies are a greater problem than ever before. Much of this is likely self-inflicted, on a broader, societal level. Some of those things, like ensuring equal rights for female trees, are within our control to do something about. The same could be said for pollution. Other things, like how your genes make you respond to these things, are not. They are what they are.
But understanding your genetic risks may also go a long way in helping you decide what steps to take to deal with your allergies. Genetics can help you focus on which strategies are more likely to work for you based on your DNA.
Maybe you have that IL13 variant that can worsen your allergies. If that’s your case, then supplementing with probiotics may help you mitigate your symptoms. The SelfDecode Allergies Report allows you to optimize your health by uncovering what your genes are doing behind the scenes to affect your odds of struggling with allergies.
SelfDecode can help you find out if you have interleukin variants that affect your getting or controlling asthma. Or maybe you have a variant in the TGFB1 gene that makes you more susceptible to asthma from air pollution. Without the knowledge, you don’t have the power to take appropriate action.
SelfDecode analyzes over 2,400 genetic variants related to allergies to give you the most precise data on your personalized report.
Unlike other DNA companies, SelfDecode goes a step beyond merely highlighting your genetic risk for allergies. Your report also comes with evidence-based diet, supplement, and lifestyle recommendations to help you optimize your defense against them.
For example, if you find out you have that STAT6 gene variant linked to higher odds of allergies, you may want to try acupuncture to help lower STAT6 activity.
SelfDecode gives you a list of personalized and prioritized health recommendations based on your DNA and aimed at improving your quality of life. SelfDecode offers over 28 wellness reports covering a wide variety of health topics, including eczema, psoriasis, and gut health.
Concluding Remarks About Allergies And Genetics
Having allergies can make you experience mild symptoms like itching, runny nose, or sneezing, but it can also present more serious reactions. Beyond this, allergies can also make you less productive and fatigued.
We’ve explained the relationship between allergies and genetics. But knowing if your allergies are genetic is just the first step. Be proactive and start today by investigating your DNA. For a gene-based approach to allergies, you should check out SelfDecode.
Related Articles
- Is IBS Genetic? Types, Risks & How To Deal
- Butterbur and Allergies: Can It Help With Hay Fever (Rhinitis)?
- What Does Lactose Intolerance Feel Like?